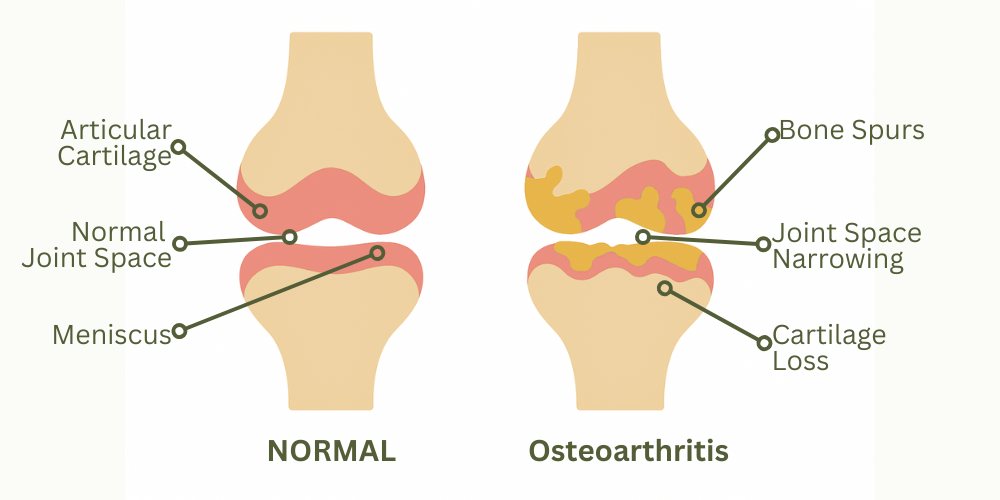
Osteoarthritis (OA) is a degenerative joint disease characterized by the breakdown of cartilage, changes in the underlying bone, inflammation, and eventual joint dysfunction. It primarily affects weight-bearing joints like the knees, hips, and spine. Preventing and managing the onset of osteoarthritis through diet and supplementation is entirely possible, but first, it’s essential to understand the key mechanisms that contribute to its development.
The Role of Calcium in Osteoarthritis
Calcium is essential for bone strength and density, and its regulation plays a key role in maintaining joint health. However, its effects on osteoarthritis can be complex:
- Bone Spurs (Osteophytes):
- In OA, calcium deposition in the joints can lead to bone spurs (osteophytes), which are small bony growths that form along joint edges. These contribute to pain, stiffness, and reduced mobility.
- This excessive calcium buildup may occur due to the body’s attempt to stabilize damaged joints and due to the deficiency in certain minerals preventing uptake of calcium into the bone itself.
- Cartilage Calcification (Chondrocalcinosis):
- In some osteoarthritis (OA) patients, tiny calcium crystals build up in the cartilage. This condition is called chondrocalcinosis. These crystals can make joint inflammation worse and speed up cartilage damage.
- Calcium is important for strong bones. But when too much calcium is floating around in the bloodstream instead of being stored in bones, it can’t be used properly by muscles. Instead, it causes problems in the body, leading to imbalance and damage.
- Calcium and Bone Health:
- Inadequate calcium uptake by the body can lead to osteoporosis, which weakens bones and increases the risk of fractures. While OA itself does not directly cause osteoporosis, both conditions can coexist, especially in aging individuals.
- Even when there is plenty of free calcium in the bloodstream, it may not be properly absorbed and deposited in bones if essential minerals, such as magnesium and phosphorus, are lacking. This imbalance can lead to symptoms of calcium deficiency despite sufficient overall calcium levels.
- This is why excessive calcium supplementation without proper regulation can lead to vascular calcification, which may contribute to inflammation and poor circulation in joints.
The Role of Magnesium in Osteoarthritis
Magnesium is critical for bone strength, muscle relaxation, and inflammatory control. Its relationship with OA includes:
- Cartilage Protection:
- Magnesium helps regulate calcium transport and prevents excessive calcium deposition in soft tissues, reducing the risk of chondrocalcinosis.
- It supports the function of chondrocytes (cartilage cells), reducing oxidative stress and inflammation that contribute to OA progression.
- Inflammation Control:
- Magnesium has anti-inflammatory properties by regulating cytokines and reducing oxidative stress. Low magnesium levels are associated with higher levels of pro-inflammatory markers, which can worsen OA symptoms.
- It also plays a role in preventing synovial membrane inflammation, which is crucial for joint lubrication.
- Muscle and Nerve Function:
- Magnesium is necessary for muscle relaxation. Since muscle tension around affected joints can increase pain and stiffness in OA, adequate magnesium levels help maintain better muscle-joint coordination.
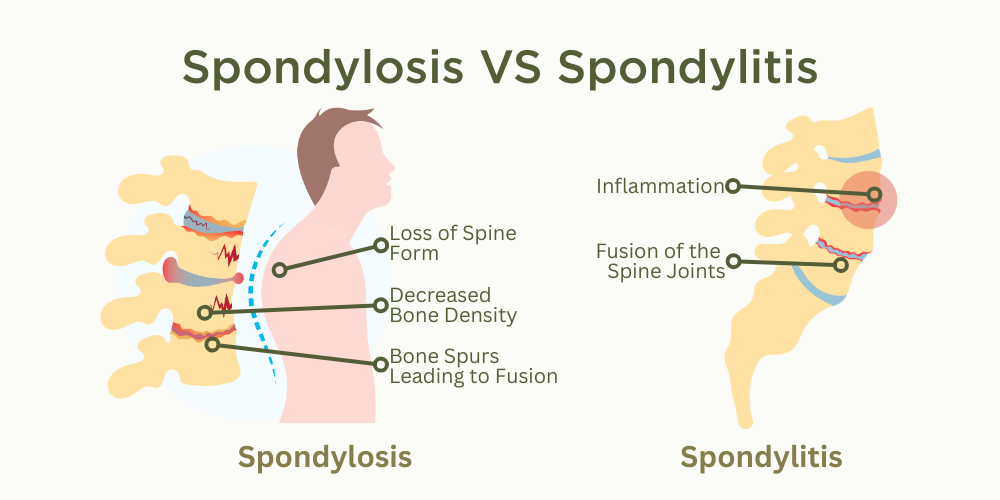
Osteoarthritis, Spondylosis, and Spondylitis
Spondylosis and Its Connection to Osteoarthritis
Spondylosis refers to degenerative changes in the spine, including OA of the vertebral joints. It is often used interchangeably with spinal osteoarthritis.
- Calcium’s Role in Spondylosis:
- Excessive calcium deposits can lead to bone spur formation on the vertebrae, contributing to nerve compression and pain.
- Disc degeneration in OA can also lead to changes in calcium metabolism, affecting spine stability.
- Magnesium’s Role in Spondylosis:
- Magnesium deficiency can lead to increased muscle tension and spasms, worsening spinal stiffness and pain.
- It also plays a role in preventing calcification of soft tissues, which can help in maintaining spinal flexibility.
Spondylitis vs. Osteoarthritis
Unlike OA, spondylitis refers to inflammatory conditions affecting the spine, such as ankylosing spondylitis (AS). This autoimmune disorder leads to chronic inflammation, fusion of vertebrae, and loss of spinal mobility.
- Calcium’s Role in Spondylitis:
- In severe cases, chronic inflammation can lead to bone overgrowth and fusion (ankylosis), often worsened by abnormal calcium metabolism.
- Patients may experience low bone density due to chronic inflammation, increasing the risk of fractures.
- Magnesium’s Role in Spondylitis:
- Magnesium helps reduce inflammation and muscle stiffness, which is beneficial in managing symptoms of spondylitis.
- It may help prevent excessive calcium deposition that leads to spinal rigidity.
Calcium and magnesium are essential for maintaining strong bones and healthy joints. When calcium levels are imbalanced, it can lead to bone spurs, cartilage calcification, and increased joint stiffness, particularly in osteoarthritis (OA) and spondylosis. A lack of magnesium further worsens these issues by promoting inflammation, muscle tightness, and improper calcium deposition. In conditions like spondylitis, which affects the spine, maintaining the right balance of these minerals is crucial for managing bone formation and reducing inflammation.
Maintaining a balanced intake of both minerals, along with vitamin D and other joint-supporting nutrients, is essential for preventing and managing OA, spondylosis, and spondylitis.

